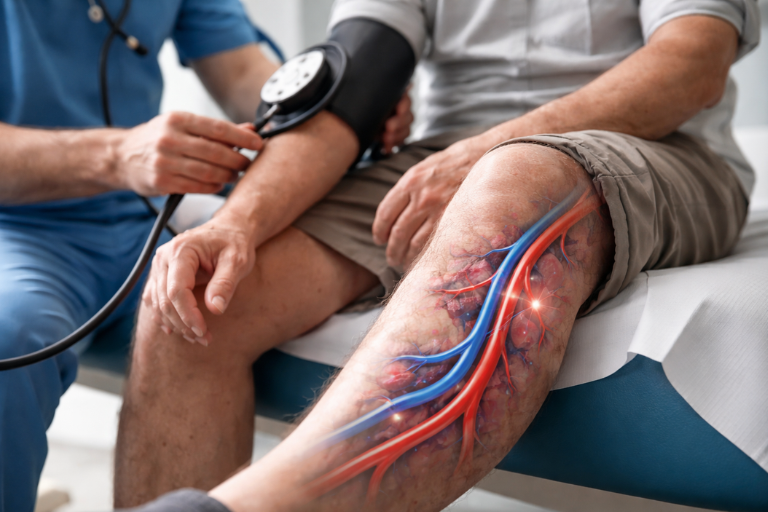
Most people who get a high blood pressure diagnosis think about their heart first. The medication. The diet changes. What rarely comes up in that first conversation is what years of uncontrolled blood pressure quietly does to the veins in the legs and what that eventually means for a wound that will not heal.
These two things are not separate coincidences happening in the same patient. One often drives the other and understanding that connection matters for anyone managing both.
Why High Blood Pressure Affects Leg Veins
Arteries carry blood away from the heart. Veins bring it back, relying on small one-way valves and leg muscle movement to keep blood flowing upward against gravity.
When blood pressure stays high for years, vein walls gradually weaken. In the legs, where blood already has to travel upward, this creates a real problem. The valves that stop blood from falling back down stop working properly. Blood pools in the lower legs. Pressure inside the veins builds. The veins stretch. This is how varicose veins form and it is directly connected to sustained high blood pressure.
How Things Get Worse Over Time
The legs stop getting enough oxygen
When blood pools in the lower legs instead of circulating properly, the surrounding tissue does not get the oxygen and nutrients it needs. Waste products build up. Fluid leaks into the tissue, which is why the ankles swell. Patients often notice this swelling first and assume it is nothing serious.
Daily habits make it worse
Long hours of sitting at a desk or standing without moving compound the problem that high blood pressure has already started. The leg muscles are what help push blood back up toward the heart, so staying still for extended periods accelerates the damage. The impact of prolonged sitting and standing on vein health is significant, especially for patients who already have elevated blood pressure.
The skin starts to change
Over time, the skin over poorly circulated areas shows the damage. Brown discoloration around the ankles, skin that feels thicker or harder, persistent redness. These are not cosmetic concerns. They are signs that the tissue underneath has been under-supplied for too long.
Why Wounds Stop Healing
This is where things become most serious.
Healing depends entirely on blood supply reaching the wound. Oxygen, immune cells and nutrients all need to get there in adequate amounts. In a leg where circulation is already compromised, that delivery is reduced before a wound even forms.
When a wound does develop, it enters a difficult environment. It takes longer to progress through the normal healing stages. Infection risk goes up because the immune response to the area is weaker. The swelling in the surrounding tissue puts additional pressure on the small blood vessels the wound needs to heal.
| Stage | What Is Happening | Effect on Healing |
| Early high blood pressure | Vein walls weaken gradually | Less elasticity in lower leg veins |
| Valve deterioration | Blood falls back and pools in the legs | Chronic pressure builds in lower leg veins |
| Established vein disease | Skin discoloration, thickening | Tissue becomes fragile, wound risk rises |
| Venous ulceration | Skin breaks down around the ankle | Healing is significantly impaired |
Venous leg ulcers, which form most often around the ankle, are the end result of this process. They are slow to heal, often taking months and they come back if the underlying vein problem is not treated alongside the wound. Understanding the difference between venous and arterial leg ulcers matters because the treatment for each is different.
What a Full Assessment Looks Like
When a patient has high blood pressure, varicose veins and a lower leg wound that is not healing, a proper evaluation covers more than a visual check.
It typically includes an ultrasound to identify where vein valves have failed, a circulation test to check whether arterial disease is also contributing, a detailed wound assessment and a review of medications, since some blood pressure drugs affect leg circulation in ways relevant to wound healing.
Treating the wound without addressing the vein problem underneath it rarely works long term. And treating the veins without managing blood pressure properly leaves the root cause in place.
How Treatment Works
Compression
Graduated compression reduces pressure in the lower leg veins, brings swelling down, improves circulation to the tissue, and helps wounds heal faster. It needs to be matched to the patient carefully, especially when arterial disease is also present.
Vein treatment
For patients with significant valve failure, treating the veins directly, through procedures like endovenous ablation or sclerotherapy, addresses the source of the problem. Clinical evidence consistently shows better wound healing outcomes when the underlying vein condition is treated as part of the care plan rather than separately.
Blood pressure control
Keeping blood pressure well managed slows the ongoing damage to vein walls. It does not undo existing valve failure, but it protects the veins that are still functioning and reduces the risk of further deterioration.
If you have high blood pressure, visible vein changes in your legs, or a wound that is taking longer than expected to heal, getting a proper vascular assessment is the right next step. At Prime Vascular Care, these conditions are evaluated together, not in isolation. Book a consultation to understand what is driving the problem and what can be done about it.